One of the marks of the globalized world is the reduction of world distances, through increasingly faster transport and the progressively optimized transmission of information at a transcontinental level. In this context, given the global technological advance, one of the areas benefited is telemedicine. Originating in Israel, it encompasses any medical practice carried out at a distance, from screening, guidance, consultation, ICU monitoring and even robotic surgeries.
In a socially unequal country like Brazil, telemedicine appears as an option to reduce such differences and boost the health area. Among its characteristics, the technology allows patients not to spend long journeys until care, reduces costs, minimizes medical conduct errors by providing small towns with access to specialists, and, mainly, unburdens Emergency Rooms so that face-to-face care can dedicate more efforts to more serious cases, acquiring special relevance in times of fighting Covid-19.
On the other hand, Brazilian medical class entities raise some concerns regarding points involving Ethics and Law, anchored in the "Declaration of Tel Aviv", the first document of international relevance on telemedicine to address such issues. Among the main fears are the traffic of confidential patient information on the network, the humanity of the care, the training of professionals in the field of telemedicine and also the impact on the labor market of these health agents. All these relevant issues, however, have been responsible for a regulatory imbroglio and slowness that has lasted for almost two decades
History of Regulation in Brazil
Created in 1951, the Federal Council of Medicine (CFM) is an autarchy that has constitutional attributions of inspection and standardization of medical practice. Therefore, the creation of norms for the scope of telemedicine fits within the constitutional roles of the council, a power that came to be exercised in this area for the first time 3 years after the "Declaration of Tel Aviv", in 2002.
Thus, the first regulation on the subject in the country became the 2002 CFM Resolution, which legally defined telemedicine as "the practice of Medicine through the use of interactive audiovisual and data communication methodologies, with the objective of assistance, education and research in Health". Furthermore, some initial steps were taken towards the regulatory advancement of Brazilian telemedicine, albeit in a broad way. Among its main points are: permission for diagnostic and therapeutic support in emergency cases, but without further specifications; the institution that responsibility for care falls to the doctor; and the duty to have "adequate technological infrastructure".
Even though it was only published in 2002, when Brazil and the world were at a very different technological level from today, the Resolution was relevant, because a "modernized" version of telemedicine regulation only came more than a decade later, in 2018, but it ended up being revoked 20 days after its implementation, returning to what had been in place since 2002. The reason for this is that the new version (2018 CFM Resolution) took a bigger step towards the intermediation of technology in medical practice, bringing the possibility of conducting teleconsultation (the probable flagship of telemedicine), albeit with rules.
In this way, with the return to the 2002 Resolution, which had not accompanied the technological reality of the country for some time, Brazil returned to having regulatory issues to be defined even until mid-March 2020, in the midst of an escalation in the number of deaths and infected by Covid-19. In this scenario, independent initiatives from what was foreseen in the regulation multiplied, such as remote "pre-consultations" and "guidance", both in the public and private sectors, to avoid the unnecessary displacement of patients to health centers and hospitals.
In the meantime, on March 19, the CFM released Resolution 2020, which recognizes the possibility of some telemedicine modalities, on an exceptional basis and solely during the pandemic, addressing teleorientation, telemonitoring and tele-interconsultation (communication between professionals on medical issues).
Responding to the demands of the state of public calamity, one day after the CFM resolution, the Ministry of Health issues Ordinance No. 467, which, also on an exceptional basis due to the pandemic, recognizes the possibility of using telemedicine for consultation and diagnosis. On April 15, Law No. 13,989 was sanctioned, which legally and definitively authorizes telemedicine, in its broad sense, as long as the health crisis persists.
Market and trend
In Brazil, an average of 150 million people depend on the SUS, which ends up generating an overload of the public health system, which in turn leads to long waiting times. Despite this problem, there is great inequality regarding the concentration of care. This is evident since more than 50% of the country's medical records are concentrated where less than a quarter of the Brazilian population lives. Together, these disparities represent great opportunities for improvement that can be supplied by the correct uses of telemedicine, as projects like Regula+Brasil were already doing.
Thus, amidst this situation, Guilherme Hummel, scientific coordinator of the Healthcare Information and Management Systems Society, stated at the beginning of 2019 that a significant amount of resources was expected to be mobilized for the development of telemedicine (between US$ 7 billion and US$ 8 billion in the next 5 years), even before any sign of the pandemic. Now, with the shock caused by the new coronavirus, investments should exceed the expert's expectation, given that not only private health centers and technology companies, but also the SUS itself, have already applied resources to create telemedicine platforms, concurrently with the growth in the search for this medical modality by internet users (as evidenced in the graph below).
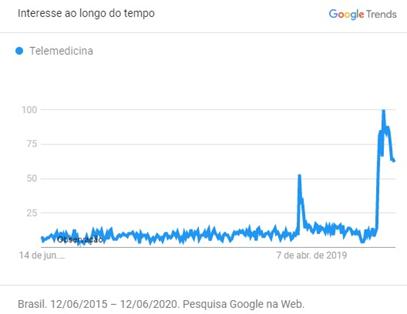
Therefore, it is to be expected that, due to society's interaction with the disruptive combination of medicine and technology, there will be an alignment process on the part of legislative and regulatory entities of medical practice, opening ground for its development. In this context, it becomes probable that telemedicine will become part of the highly prophesied "new normal" in which we will be inserted in the post-pandemic.